What is a dental implant?
A dental implant is a small, biocompatible titanium screw that is placed into the upper or lower jaw to replace the root of a missing tooth. Over time, your bone heals and bonds directly to the implant through a process called osseointegration, creating a strong and stable foundation for a new tooth.
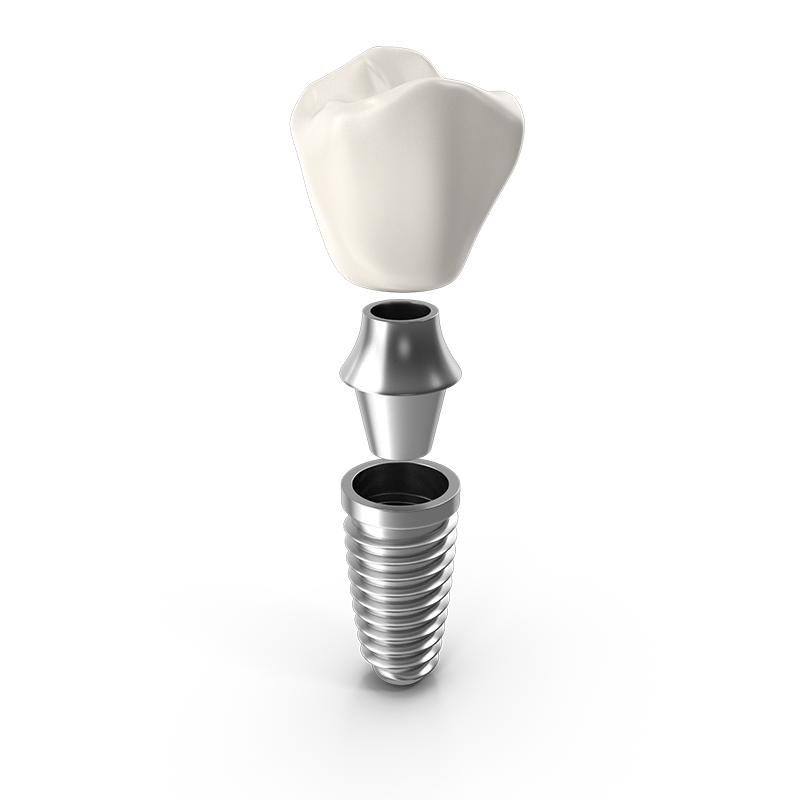
Titanium Implant
Your oral surgeon places this piece into your jawbone. It acts as your new tooth root.Abutment
This is the support post, connecting the implant to the crown.Crown
Your dentist will create this crown, designed to match the rest of your teeth in color and size for the most natural appearance.Most implant restorations have three parts:
- Implant – the titanium “root” placed in the bone
- Crown – the visible tooth, made by your restorative dentist
- Abutment – the connector between the implant and crown
The goal is simple: to replace a missing tooth in a way that looks natural, feels secure, and functions like your own tooth.
Why are implants a great option?
Dental implants are considered one of the most important advances in modern dentistry. They allow us to replace missing teeth in a way that closely mimics natural anatomy and function.
Common benefits include:
- High long-term success rates when properly planned and maintained
- No need to cut down neighboring teeth, as required with traditional bridges
- Preservation of bone, which naturally shrinks after tooth loss
- Improved function, comfort and stability
When a tooth is lost and not replaced, the surrounding bone gradually resorbs. Because an implant functions like a root, it helps stimulate and preserve that bone over time.

Evidence supporting implant success
Dental implants have decades of research behind them, including long-term follow-up studies involving thousands of patients.
Reported success rates generally range from 93–99% in healthy individuals.
- Howe MS, Keys W, Richards D. Long-Term (10-Year) Dental Implant Survival: A Systematic Review and Sensitivity Meta-Analysis. Journal of Dentistry. 2019.
- French D, Ofec R, Levin L. Long-Term Clinical Performance of 10,871 Dental Implants With Up to 22 Years of Follow-Up: A Cohort Study in 4,247 Patients. Clinical Implant Dentistry and Related Research. 2021.
These studies — along with many others — consistently demonstrate that implants are highly predictable and durable when patients are appropriately selected and properly maintained.
Bottom line: Dental implants are among the most researched treatments in dentistry, with strong long-term data supporting their use.
How do we achieve high success rates?
Implant success begins well before surgery.
- Careful Case Selection: Not every patient is automatically a candidate. We carefully review:
- Your overall medical history
- Medications
- Smoking status
- Bone quality and quantity
- Occlusion (bite) and clenching/grinding habits
- Comprehensive Exam & 3D Imaging: We evaluate the surrounding tissues and use three-dimensional imaging to assess bone volume, density, and proximity to important structures. This allows us to plan for long-term stability.
- Digital Planning & Collaboration: We use advanced planning software and coordinate closely with your restorative dentist to ensure the implant is positioned ideally for the final tooth.
- Guided Surgery & Surgical Navigation (X-Nav): In select cases, we utilize dynamic surgical navigation (X-Guide technology). This system functions similarly to a GPS for implant placement. It allows us to:
- Digitally plan implant position before surgery
- Track the drill in real time during placement
- Improve precision in angulation and depth
- Enhance predictability, especially in complex anatomy
- Long-Term Follow-Up: Implant success doesn’t end with surgery. Routine hygiene visits, monitoring, and protective nightguards when indicated all contribute to longevity.
Alternatives to dental implants
Bridge
A bridge replaces the missing tooth by placing crowns on the teeth adjacent to the space and suspending a replacement tooth between them.
Pros
- No surgery
- Can be completed relatively quickly
- Natural appearance
Cons
- Requires removing healthy neighboring teeth
- Bone beneath the missing tooth area may continue to shrink
- Hygiene can be more challenging
Implants are popular in part because they avoid these drawbacks.
Removable partial denture (“flipper”) or full denture
Pros
- Lower upfront cost
- Non-surgical
- Can replace multiple teeth
Cons
- Less stable
- May affect speech and chewing
- Can irritate gum tissue
- Requires daily removal and cleaning
- Does not prevent bone loss like a root-form implant
No replacement
Pros
- No procedure
- No cost
Cons
- Adjacent teeth may drift or tip
- Bite can change over time
- Chewing efficiency may decrease
- Progressive bone loss in the area
- Potential cosmetic concerns
Risks of implant placement
Most patients recover within a few days and are feeling back to normal after a week. However, implants are still a surgical procedure and are not risk-free.
Possible risks include:
- Swelling and discomfort
- Infection
- Implant failure (rare, but possible)
- Inflammation around the implant (peri-implant mucositis or peri-implantitis), which can lead to bone loss
- Mechanical complications such as screw loosening, component fracture, or porcelain chipping
- The need for additional procedures, including bone grafting
While complications are uncommon, long-term success depends on careful planning and ongoing maintenance.
Factors that increase risk
Long-term studies consistently identify patient-related factors that influence outcomes:
- Smoking
- Poor oral hygiene
- Uncontrolled diabetes
- Certain systemic health conditions
- Heavy clenching or grinding (bruxism)
These factors do not automatically prevent implant placement, but they require thoughtful planning and monitoring.
- Our philosophy
Dental implants are among the most researched treatments in dentistry, with strong long-term data supporting their use.
Frequently asked questions
Answers to the questions we hear most from patients.
Does getting a dental implant hurt?
Most patients find the procedure to be straightforward with manageable recovery.
Implant placement is typically done under local anesthesia, and sedation is available if needed. During the procedure, you should not feel pain. Afterward, most patients describe the discomfort as mild— often comparable to a tooth extraction.
Many people return to normal activity within two to four days.
How long does the process take?
In many cases, the implant is placed and allowed to heal for about 10-12 weeks before the final crown is made. This allows the bone to fully integrate with the implant.
If bone grafting is needed, healing time may be longer. In select cases, temporary teeth can be placed sooner.
We’ll review your specific timeline during your consultation.
How long do dental implants last?
When properly placed and well maintained, implants can last many years, decades — often a lifetime.
Long-term studies following implants for 10–20+ years show high survival rates. Like natural teeth, implants require routine hygiene visits and good home care to stay healthy.
The implant itself often lasts longer than the crown attached to it. Crowns may need replacement over time due to normal wear.
Am I a candidate for dental implants?
Most healthy adults are candidates.
Ideal conditions include:
- Adequate bone volume
- Good oral hygiene
- Controlled medical conditions
Smoking, uncontrolled diabetes, or heavy clenching may increase risk, but they do not automatically disqualify you. We evaluate each case individually.
If bone is limited, bone grafting may allow us to create a stable foundation.
What happens if I don’t replace a missing tooth?
When a tooth is not replaced:
- The surrounding bone slowly shrinks
- Adjacent teeth may drift or tip
- The bite can shift
- Chewing efficiency may decrease
Over time, this can make future treatment more complex.
What is peri-implantitis?
Peri-implantitis is inflammation and bone loss around an implant, often related to plaque buildup and poor hygiene.
It is similar to gum disease around natural teeth. Early inflammation (peri-implant mucositis) can often be reversed. Advanced bone loss is more difficult to treat.
Routine maintenance and good home care are essential to prevent this.
Are implants better than bridges?
They are different treatments with different advantages.
Implants do not require cutting down neighboring teeth and help preserve bone. Bridges avoid surgery but rely on adjacent teeth for support.
In many cases, implants are the most conservative long-term solution — but the right choice depends on your individual situation.
Can implants fail?
Yes — although it is uncommon.
Failure rates in healthy patients are low (generally reported in the 1–7% range depending on conditions). Failure can occur early (lack of integration) or later due to infection or overload.
Careful planning, proper placement, and long-term maintenance significantly reduce risk.
Do you use advanced technology during implant placement?
Yes. In appropriate cases, we use 3D imaging and dynamic surgical navigation (X-Guide technology).
This allows us to digitally plan implant placement and track positioning in real time during surgery — improving precision and predictability.

