What is the TMJ?
The temporomandibular joint (TMJ) is the joint that connects your lower jaw (mandible) to your skull. You have one on each side of your face, just in front of your ears.
It is a remarkably complex joint. It allows you to:
- Open and close your mouth
- Chew
- Speak
- Yawn
- Swallow
It functions every time you eat, talk, or even clench your teeth. Because of how often we use it throughout the day, it is one of the most active joints in the body.
What is TMD?
TMD (Temporomandibular Disorder) refers to a group of conditions that affect:
- The jaw joint
- The surrounding muscles
- The supporting structures
TMD can cause:
- Jaw pain
- Headaches
- Facial soreness
- Clicking or popping
- Locking of the jaw
- Difficulty chewing
- Ear discomfort
- Neck tension
For some patients, TMD can significantly impact quality of life — affecting sleep, eating, concentration, and overall well-being.
If you are experiencing TMJ pain, you are not alone. And it is not “just in your head.”
Understanding the anatomy
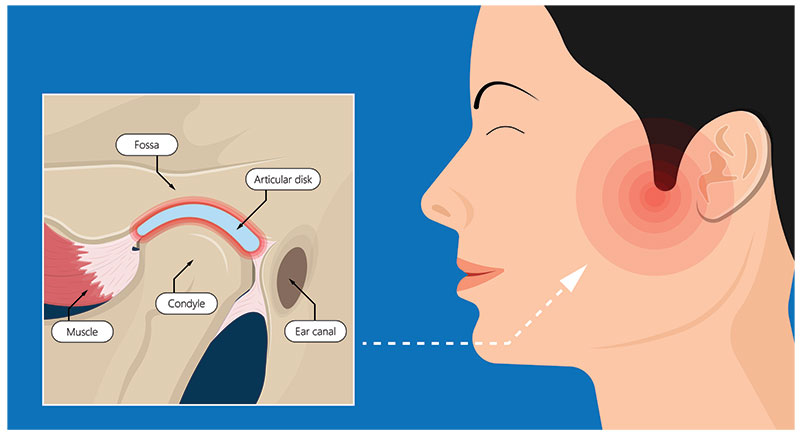
The TMJ is more complex than most joints in the body. It includes:
- The Condyle: the rounded end of the lower jaw
- The Glenoid Fossa: the socket in the skull
- The Articular Disc: a small cushion of cartilage between the condyle and fossa
The disc acts as a shock absorber and allows smooth movement.
When the disc shifts out of position, degenerates, or becomes inflamed, pain and dysfunction can occur.
Additionally, the muscles that control jaw movement — particularly the masseter and temporalis muscles — can become tight, overworked, and painful.
Often, TMD is a combination of joint mechanics and muscle tension.
Our approach to TMJ treatment
TMD is highly individualized.
There is no one-size-fits-all solution.
The most important principle: Surgery is rarely the first answer.
The vast majority of patients improve with conservative treatment.
Conservative treatment options
Pain control
Short-term use of anti-inflammatory medications can reduce joint inflammation and muscle soreness.
Muscle relaxation
Stress, clenching, and grinding play a significant role in TMD.
Addressing muscle tension is often a major component of treatment.
Night guards (occlusal splints)
Custom night guards help:
- Reduce clenching forces
- Protect teeth
- Decrease muscle overload
- Allow the joint to rest
These are often one of the most effective first-line treatments.
Physical therapy
Targeted physical therapy can improve:
- Jaw mobility
- Muscle coordination
- Postural alignment
- Neck and shoulder tension
Manual therapy and guided exercises can significantly reduce symptoms in many patients.
Botox therapy
Botox has become an effective option for patients with significant muscle-related TMD.
Botox works by:
- Reducing overactivity of the masseter and temporalis muscles
- Decreasing clenching forces
- Relieving muscle-related headaches and facial pain
It does not change your bite or jaw position. Instead, it reduces the intensity of muscle contraction.
For appropriate candidates, Botox can provide meaningful relief and improve quality of life.
Treatment is temporary and typically lasts 3–4 months.
When is surgery considered?
Surgical treatment is reserved for carefully selected cases
We’ll typically consider surgery when:
- Conservative therapy has failed
- There is structural joint damage
- Imaging confirms mechanical obstruction or degeneration
Surgical options may include:
Arthrocentesis
A minimally invasive procedure where the joint is flushed to reduce inflammation and improve movement.
Arthroplasty
A surgical procedure to repair or reposition the disc and address joint damage.
TMJ Replacement
In severe degenerative cases, the joint can be replaced with a prosthetic joint.
This is reserved for advanced disease and requires extremely careful evaluation.
The importance of proper diagnosis
TMJ disorders can be caused by:
- Muscle tension
- Disc displacement
- Degenerative joint disease
- Inflammatory conditions
- Bite imbalance
- Trauma
Correct diagnosis determines the correct treatment.
Case selection is paramount — especially when considering surgery.
- Our philosophy
TMJ disorders can be exhausting. We understand. Our approach is conservative and individualized — we start with the least invasive options and reserve surgery for when it is truly necessary.
Frequently asked questions
Answers to the questions we hear most from patients.
Is TMD permanent?
Not necessarily. Many patients improve significantly with conservative care.
Does everyone with jaw clicking need surgery?
No. Clicking alone — without pain or limitation — often does not require intervention.
Is Botox safe?
When administered appropriately, Botox is safe and well-tolerated. It is widely used for both cosmetic and therapeutic purposes. We carefully evaluate whether it is appropriate for your condition.
Can stress cause TMJ?
How long does treatment take?
It depends on the cause. Some patients improve within weeks. Others require a longer, stepwise treatment plan.

